How to Talk to Your Kids About Tobacco & E-cigarettes
It may seem difficult to talk to your kids about tobacco, especially when there are so many other dangers out there. However, this isn’t a conversation that can wait because nine out of 10 smokers start by age 18.[1] Every day in the U.S., more than 3,200 youth (18 or younger) try their first cigarette and an additional 2,100 youth and young adults become daily smokers.[2]
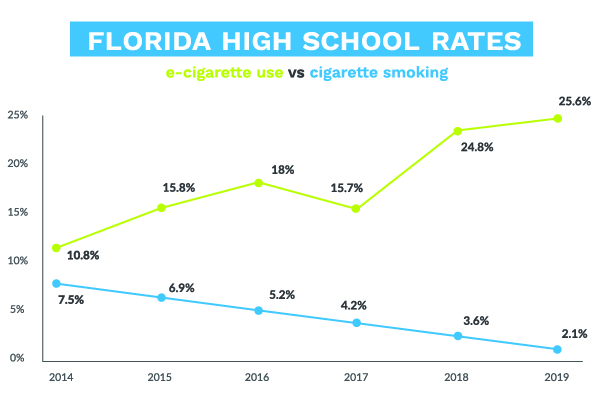
In addition, today’s youth have adopted a new type of product at an alarming rate: e-cigarettes. In 2019, 25.6% of Florida high school students reported current use of e-cigarette use, aka “vaping” – a 63% increase compared to 2017.[3]
TIPS FOR TALKING TO YOUR KIDS:

Be patient and ready to listen, encourage open dialogue and avoid criticism. Start the conversation naturally. For example, if you and your teen see someone using an e-cigarette or you walk by an e-cigarette shop, you might ask what they think to start your discussion.



Some of the most popular e-cigarette devices look like flash drives, pens, and inhalers, which can be easily concealed. Some e-cigarettes require charging, so check what devices are being charged or look for unusual plugs. If you don’t smell anything, don’t assume they aren’t using products with nicotine. E-cigarettes typically won’t make clothes smell of tobacco.


Here are some resources to start:

Are you a parent that smokes or uses tobacco?
- Research shows that kids who have a parent who smokes are more likely to smoke, and to be heavier smokers at young ages.[7] But the good news is that when parents quit smoking, their kids become less likely to start.[6]
- If you’re a parent who is ready to quit smoking, we have free tools and services that can help. Click here to sign up.
Looking for tools to help youth quit nicotine?
-
- Youth 11-13 years old can access:
- Phone Quit and receive unlimited ongoing support from a Quit Coach. The Quit Coach can also assist with assessment and planning, as well as setting a quit date.
- Youth 13-17 years old can choose from:
- Phone Quit – Calls with a Quit Coach to help with assessment and planning, as well as setting a quit date.
- Web Quit – Stand-alone online program that allows the user to chat with a Quit Coach.
- Youth 11-13 years old can access:
You can help by educating yourself, dispelling myths among your friends and family, and talking to your kids about the serious concerns around vaping and nicotine addiction.
For additional tips, take a look at the Surgeon General’s tip sheet for parents here.
_______________________________________________________________________________________________________________________________________________________
[1] U.S. Department of Health and Human Services. (2014). The Health Consequences of Smoking—50 Years of Progress: A Report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health.
[2] U.S. Department of Health and Human Services. The Health Consequences of Smoking: 50 Years of Progress. A Report of the Surgeon General. Atlanta, GA: U.S. Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Chronic Disease Prevention and Health Promotion, Office on Smoking and Health, 2014. Printed with corrections, January 2014.
[3] Florida Youth Tobacco Survey (FYTS), Florida Department of Health, Bureau of Epidemiology, 2019.
[4] Newman, I, et al., “The influence of parental attitude and behavior on early adolescent cigarette smoking,” Journal of School Health 59(4):150-2, April 1989. See also, Distefan, J, et al., “Parental influences predict adolescent smoking in the United States, 1989-1993,” Journal of Adolescent Health 22:466-74, 1998.
[5] Adachi-Mejia, A. M., Gibson Chambers, J. J., Li, Z., & Sargent, J. D. (2014). The relative roles of types of extracurricular activity on smoking and drinking initiation among tweens. Academic pediatrics, 14(3), 271-8.
[6] Gilman, SE, et al., “Parental Smoking and Adolescent Smoking Initiation: An Intergenerational Perspective on Tobacco Control,” Pediatrics 123(2): e274-e281, February 2009. Bauman, K, et al., “Effect of parental smoking classification on the association between parental and adolescent smoking,” Addictive Behaviors 15(5):413-22, 1990. See also, Osler, M, et al., “Maternal smoking during childhood and increased risk of smoking in young adulthood,” International Journal of Epidemiology 24(4):710-4, August 1995.
[7] Wyszynski, C. M., Bricker, J. B., & Comstock, B. A. (2011). Parental smoking cessation and child daily smoking: A 9-year longitudinal study of mediation by child cognitions about smoking. Health psychology: official journal of the Division of Health Psychology, American Psychological Association, 30(2), 171-6.